Understanding Prostate Health and Its Impact on Men
Nearly 50% of men will experience some form of prostate-related complaint by age 60, and that number rises sharply with each passing decade. Yet despite how widespread these concerns are, most men have only a vague sense of what the prostate actually does, what goes wrong with it, and what realistic options exist. Taking time to understand prostate health isn’t just academic; it directly shapes the decisions men make about screening, lifestyle, and supplementation.
This guide covers what the prostate is, the conditions that affect prostate health most, warning signs worth knowing, and practical strategies, including a closer look at how a well-formulated supplement fits into a broader wellness routine.
Key Takeaways
| Question | Answer |
|---|---|
| What does the prostate actually do? | It produces seminal fluid that nourishes sperm. Its location wrapping around the urethra means enlargement directly disrupts urination. |
| At what age should men start paying attention? | Awareness should begin in the 40s. Routine screening discussions with a doctor are appropriate from age 50, or earlier with risk factors. |
| What are the three most common prostate conditions? | BPH (benign enlargement), prostatitis (inflammation), and prostate cancer, each with distinct symptoms and management approaches. |
| Can lifestyle genuinely make a difference? | Yes. Diet, exercise, weight management, and targeted supplementation all have documented effects on markers of prostate health. |
| What symptoms should never be ignored? | Blood in urine, inability to urinate, bone pain, or sudden dramatic PSA increases warrant prompt medical evaluation. |
| How does a multi-ingredient supplement help? | Formulas like Prost-Fix address multiple pathways simultaneously, hormone balance, inflammation, antioxidant defense, and nutritional support. |
1. What the Prostate Is and Why It Matters
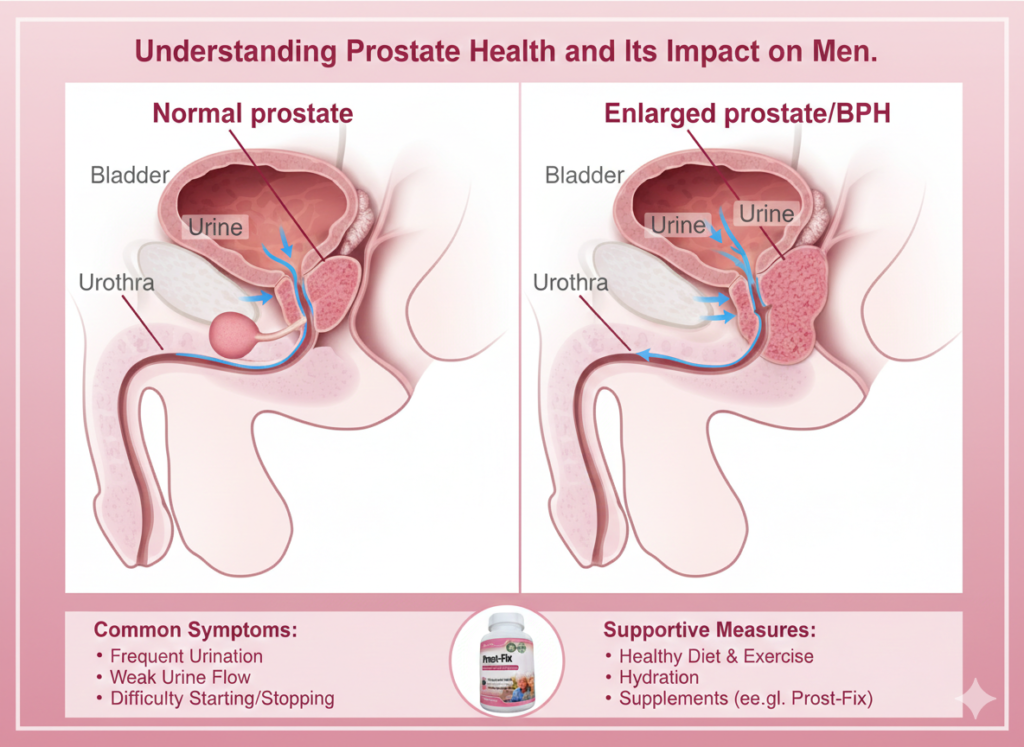
The prostate is a walnut-sized gland sitting just below the bladder, surrounding the urethra. Understanding prostate health begins with this anatomy: because the gland wraps around the urethra, even modest swelling creates outflow obstruction. Men experience this as a weak stream, incomplete emptying, or frequent nighttime trips to the bathroom, symptoms collectively called lower urinary tract symptoms (LUTS).
The prostate also responds to hormones, particularly testosterone and its more potent metabolite dihydrotestosterone (DHT). This hormonal sensitivity is central to most age-related changes and is a key target for both pharmaceutical and natural interventions.
2. Three Conditions That Affect Prostate Health Most
1: Benign Prostatic Hyperplasia (BPH)
BPH is the most common prostate condition, affecting around 50% of men in their 50s and up to 90% of men in their 80s. The gland enlarges as part of normal aging, driven partly by rising estrogen-to-testosterone ratios and continued DHT stimulation. Supporting prostate health through nutrition and supplementation is most practical when begun before symptoms become severe.
BPH itself is not cancerous and doesn’t raise cancer risk directly. However, its symptoms, urgency, frequency, weak flow, and nocturia, erode sleep quality and daily comfort. The International Prostate Symptom Score (IPSS) quantifies severity, with scores above 8 indicating moderate-to-severe symptoms.
2: Prostatitis
Prostatitis is inflammation of the gland, more common in younger and middle-aged men than BPH. It presents in four forms, ranging from acute bacterial infection (requiring antibiotics) to chronic pelvic pain syndrome, the most prevalent and hardest-to-treat variant.
Men with chronic prostatitis report pelvic pain, discomfort with urination or ejaculation, and reduced quality of life. Anti-inflammatory nutrients and botanical compounds show promise for symptom relief in this group.
3: Prostate Cancer
Prostate cancer is the most diagnosed non-skin cancer in American men, with approximately one in eight men receiving this diagnosis in their lifetime. It is also one of the most survivable cancers when detected early, five-year survival rates exceed 99% for localized disease.
PSA (prostate-specific antigen) testing remains the primary screening tool despite ongoing debate about optimal intervals. Men at elevated risk, those with a family history or of African-American descent, are typically advised to begin screening discussions with their doctor by age 40-45.
Did You Know? The risk of a man developing BPH increases by roughly 4% for every year of life after 40. By age 85, almost all men show some degree of prostatic enlargement on imaging, though not all experience bothersome symptoms.
3. Recognizing Symptoms: When to Pay Attention
Many men normalize prostate-related symptoms because they develop gradually. Understanding which changes are worth monitoring, and which demand urgent attention, is a core part of managing prostate health proactively.
Common Symptoms to Monitor
- Needing to urinate more than once at night (nocturia)
- Weak, interrupted, or slow urinary stream
- Difficulty starting urination despite feeling the urge
- Sensation of incomplete bladder emptying
- Increased urgency or frequency during the day
- Dribbling after urination
These symptoms are consistent with BPH and chronic prostatitis and are generally not emergencies, though they warrant evaluation.
Symptoms Requiring Prompt Medical Attention
- Blood in urine or semen
- Severe or sudden inability to urinate
- Unexplained weight loss paired with urinary changes
- Pain in the lower back, hips, or pelvis (a potential sign of advanced disease)
- Rapidly rising PSA on consecutive tests
Any of these warrant prompt medical evaluation rather than a watchful waiting approach.
4. Lifestyle Factors That Directly Shape Outcomes
Prostate health is not purely genetic or inevitable. Modifiable lifestyle factors have documented, measurable effects on gland size, inflammatory markers, and symptom severity.
Diet
A plant-forward diet consistently correlates with better prostate health outcomes across populations. Foods with the strongest evidence include tomatoes (lycopene), cruciferous vegetables (sulforaphane), fatty fish (omega-3s), green tea (EGCG catechins), and pumpkin seeds (zinc and phytosterols).
Conversely, diets high in processed meats and refined carbohydrates are associated with higher rates of BPH and more aggressive disease in observational studies.
Exercise
Regular aerobic and resistance exercise reduces systemic inflammation, supports healthy testosterone metabolism, and helps maintain body weight, all of which benefit the gland. One meta-analysis found that men who exercised regularly had IPSS scores approximately 3 points lower than sedentary men, meeting the threshold for a clinically meaningful difference.
Body Weight and Stress
Obesity directly affects hormone metabolism, raising estrogen relative to testosterone and increasing inflammation. Weight loss in overweight men reduces prostate volume and improves urinary flow in clinical studies. Chronic stress compounds this by elevating cortisol and disrupting hormone balance, amplifying symptoms further.
Did You Know? Physically active men have a 25-30% lower risk of developing symptomatic BPH compared to sedentary men, according to a long-term cohort study published in the Journal of Urology.
5. Natural Compounds with Clinical Evidence
Several plant-based compounds have been studied specifically for their effects on the gland, urinary symptoms, and inflammatory markers. Men focused on prostate health through natural means will find consistent evidence for the following:
Saw palmetto (Serenoa repens): The most widely studied herb for BPH, with modest evidence supporting improvements in urinary flow and symptom scores. Large trials show mixed results, but tolerability is excellent.
Beta-sitosterol: A plant sterol with relatively strong clinical data. Meta-analyses show meaningful improvements in IPSS and peak urinary flow, exceeding the minimal clinically important threshold of a 3-point IPSS drop.
Pygeum bark: Pygeum africanum extract shows one of the more consistent clinical signals among prostate herbs, with IPSS improvements of around 38% at two months in controlled trials.
Nettle root: Influences sex hormone-binding globulin and inflammatory pathways; pairs well with saw palmetto in European formulations.
Zinc: The gland concentrates zinc more than almost any other tissue. Men with BPH often show significantly depleted tissue zinc, and supplementation may support normal function.
Quercetin: Shows particular promise for chronic prostatitis, reducing pain scores and improving quality of life in randomized trials.
No single compound works dramatically on its own, the research on prostate health consistently points toward combinations addressing multiple pathways simultaneously.
6. Spotlight on Prost-Fix: A 30-Ingredient Formula for Complete Prostate Health Support
Understanding the evidence behind individual ingredients leads naturally to a practical question: how do you actually implement all of this? Managing six separate supplements is expensive, easy to forget, and difficult to dose accurately. This is exactly the problem Prost-Fix was designed to solve—providing comprehensive prostate health support in one convenient capsule.
Developed with a Medical Research Foundation
Prost-Fix was formulated under the guidance of William Anderson, a medical researcher specializing in men’s health. The formula reflects current evidence on what prostate health requires, not marketing trends or ingredient cost-cutting.

30 Ingredients Across Six Pathways
Rather than loading up on one or two headline herbs, Prost-Fix addresses six distinct biological pathways:
Hormone balance: Saw palmetto, nettle root, and beta-sitosterol modulate DHT activity and estrogen metabolism, targeting the hormonal drivers of BPH.
Inflammation control: Quercetin, pomegranate extract, and turmeric work together to lower inflammatory cytokines that contribute to gland swelling and discomfort.
Antioxidant defense: Selenium, vitamin E, green tea extract, and lycopene protect gland tissue from the oxidative damage that accumulates with age.
Nutritional support: Zinc picolinate and vitamin B6 (as P5P) provide essential nutrients that the gland relies on for normal metabolic function, both commonly depleted in men with BPH.
Urinary comfort: Pumpkin seed extract, flower pollen, and amino acids (L-alanine, glycine) support bladder neck tone and urinary flow.
Immune modulation: Vitamin D3, selenium, and zinc work synergistically to maintain balanced immune responses in gland tissue.
Why Combination Outperforms Single Ingredients
Prostate health problems rarely stem from just one cause. BPH involves hormonal shifts, inflammation, oxidative stress, and nutritional deficits happening simultaneously. Addressing only one pathway, as a single-herb supplement does, leaves the others unchecked.
Prost-Fix brings these pathways together in one small capsule, making daily consistency achievable. Men typically begin noticing improvements in urinary symptoms within four to eight weeks, with fuller benefits emerging over three to six months of consistent use.
What Prost-Fix Is Not
It’s worth being direct: Prost-Fix is a nutritional support formula, not a pharmaceutical drug. It will not produce the rapid, dramatic changes that alpha-blockers or 5-alpha reductase inhibitors can achieve for severe BPH. For men with significant symptoms or elevated PSA, medical evaluation should come first.
What it can do, and what the evidence for its individual ingredients supports, is provide meaningful, sustained nutritional and botanical support as part of a proactive prostate health strategy.
Prost-Fix Pricing and Supply Options
| Option | Supply Length | Price | Notes |
|---|---|---|---|
| Prost-Fix – 1 Bottle | 30-day supply | $29.95 | A practical starting point to assess your individual response. |
| Prost-Fix – 3 Bottles | 90-day supply | $59.90 | Best value for the three-to-six-month window where full benefits develop. |
7. Routine Monitoring: The Role of Screening
Lifestyle and supplementation are most valuable when paired with appropriate medical monitoring. Maintaining prostate health long-term requires knowing your numbers.
PSA testing: PSA is not a perfect test, but it remains the best available screening tool. A rising trend over time is more significant than any single absolute number. Men should discuss testing intervals with their doctor rather than either ignoring PSA or overreacting to minor fluctuations.
Annual examinations: A digital rectal exam (DRE) provides information about gland size and texture that PSA alone cannot.
Symptom tracking: The IPSS questionnaire takes two minutes to complete. Tracking your score every three to six months provides objective data on whether symptoms are stable, improving, or worsening.
Conclusion
Prostate health affects nearly every man eventually, but it is far from an inevitability that must simply be endured. Understanding your own prostate health, recognizing early warning signs, making evidence-informed lifestyle changes, and choosing well-formulated nutritional support, contributes to meaningfully better outcomes.
The evidence points consistently toward a multi-pathway approach: diet, exercise, stress management, appropriate screening, and targeted supplementation working together. Formulas like Prost-Fix are most valuable when they complement this foundation, not substitute for it.
Men who monitor symptoms, maintain open communication with their healthcare providers, and act early consistently achieve better quality of life as they age than those who wait for problems to become severe.